Blog Post Title: Fertility Medications vs Surgery: A Comparison of Side Effects and Risks
Introduction:
Fertility issues can be a source of stress and frustration for many couples trying to conceive. Fortunately, there are various treatment options available, including fertility medications and surgery. These methods are designed to help regulate hormones, improve ovulation, and increase the chances of pregnancy. However, both options come with their own set of side effects and risks. In this blog post, we will take a closer look at fertility medications and surgery, comparing the potential side effects and risks associated with each.
Fertility Medications:
Fertility medications are drugs that are used to help stimulate ovulation and increase the chances of getting pregnant. They work by regulating hormones and stimulating the ovaries to produce and release eggs. Some common fertility medications include Clomid, Letrozole, and Gonadotropins.
Side Effects:
While fertility medications can be effective in helping couples conceive, they also come with potential side effects. Some of the most common side effects include hot flashes, mood swings, headaches, and bloating. These side effects are usually mild and temporary, but they can still cause discomfort and affect daily activities. In some cases, fertility medications can also increase the risk of developing ovarian hyperstimulation syndrome (OHSS), a condition where the ovaries become swollen and painful.
Risks:
Aside from side effects, fertility medications also come with potential risks. One of the main concerns is the increased risk of multiple pregnancies. This is because fertility drugs can stimulate the ovaries to release more than one egg, increasing the chances of conceiving twins, triplets, or even more. Multiple pregnancies come with a higher risk of complications, such as premature birth and low birth weight. Fertility medications can also increase the risk of ectopic pregnancy, where the fertilized egg implants outside of the uterus.
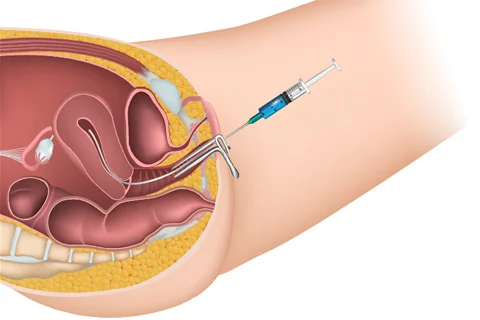
Surgery:
In some cases, fertility issues may require surgery to correct underlying problems. This can include procedures such as laparoscopy, hysteroscopy, or tubal ligation reversal. These surgeries are designed to address issues such as blocked fallopian tubes, endometriosis, or uterine abnormalities.

Fertility Medications vs Surgery: A Comparison of Side Effects and Risks
Side Effects:
Similar to fertility medications, surgery also comes with potential side effects. These can include pain, bleeding, infection, and scarring. The severity of these side effects can vary depending on the type of surgery and individual factors. For example, laparoscopy is a minimally invasive procedure, which means it has a lower risk of side effects compared to more invasive surgeries.
Risks:
Surgery also carries the risk of complications, such as damage to surrounding organs or tissues. In rare cases, surgery can also lead to fertility problems, such as scarring or damage to the fallopian tubes. Additionally, surgery may not always be successful in addressing fertility issues, requiring further procedures or treatments.
Comparison:
When it comes to comparing fertility medications and surgery, there are several factors to consider. Both options come with potential side effects and risks, but the severity and likelihood of these vary. Fertility medications have a higher risk of multiple pregnancies, while surgery carries a higher risk of complications and may not always be successful.
Another aspect to consider is the cost. Fertility medications are generally less expensive compared to surgery, which can be a significant factor for those with limited financial resources. However, in some cases, surgery may be the more cost-effective option in the long run, especially if fertility medications are not successful or multiple procedures are needed.
It is also essential to consider personal preferences and medical history. Some individuals may prefer to try fertility medications first before considering surgery, while others may opt for surgery right away. Additionally, certain medical conditions may make one option more suitable than the other.
Conclusion:
In the end, the decision between fertility medications and surgery comes down to individual circumstances and preferences. Both options have their own set of side effects and risks, and it is essential to weigh them carefully before making a decision. Consulting with a trusted healthcare provider can also help in determining the best course of action for each individual’s unique situation.
In summary, fertility medications and surgery are two treatment options available for couples struggling with fertility issues. While both can be effective in helping achieve pregnancy, they also come with their own set of side effects and risks. It is important to consider factors such as cost, personal preferences, and medical history when deciding between the two options. Consulting with a healthcare provider can also help in making an informed decision.