Blog Post:
When it comes to fertility issues, there are various treatment options available, including fertility medications and surgery. These two methods have been proven to be effective in helping couples conceive, but they have different approaches and outcomes. Choosing between fertility medications and surgery can be a daunting decision, and it is essential to make an informed choice. In this blog post, we will explore the differences between these two methods and provide some helpful tips on how to make the best decision for your fertility journey.
Fertility Medications:
Fertility medications are often the first line of treatment for couples struggling with infertility. These medications are designed to stimulate ovulation, regulate hormones, and improve the quality and quantity of eggs produced. They are available in different forms, including pills, injections, and nasal sprays, and are prescribed based on the underlying cause of infertility.
One of the most commonly prescribed fertility medications is Clomiphene citrate (Clomid), which stimulates the release of hormones that trigger ovulation. Other medications, such as Gonadotropins and Metformin, are also used to stimulate ovulation and regulate insulin levels in women with polycystic ovary syndrome (PCOS).
Pros of Fertility Medications:
1. Non-invasive: Fertility medications are taken orally or through injections, making them less invasive compared to surgery.
2. Cost-effective: Medications are generally more affordable than surgery, making them a more accessible option for many couples.
3. Fewer side effects: While fertility medications may cause some side effects, they are usually mild and easily manageable.
4. Can be used for a longer duration: Fertility medications can be used for several cycles, giving couples more chances to conceive without undergoing surgery.
Cons of Fertility Medications:
1. Limited success rates: Fertility medications may not work for everyone, and success rates vary depending on the underlying cause of infertility.
2. Multiple pregnancies: Some fertility medications may increase the chances of conceiving multiples, such as twins or triplets, which can lead to a high-risk pregnancy.
3. Ovarian hyperstimulation syndrome (OHSS): In some cases, fertility medications can overstimulate the ovaries, leading to OHSS, a potentially serious condition that can cause bloating, abdominal pain, and shortness of breath.
Surgery:
Fertility Medications vs Surgery: How to Make an Informed Decision
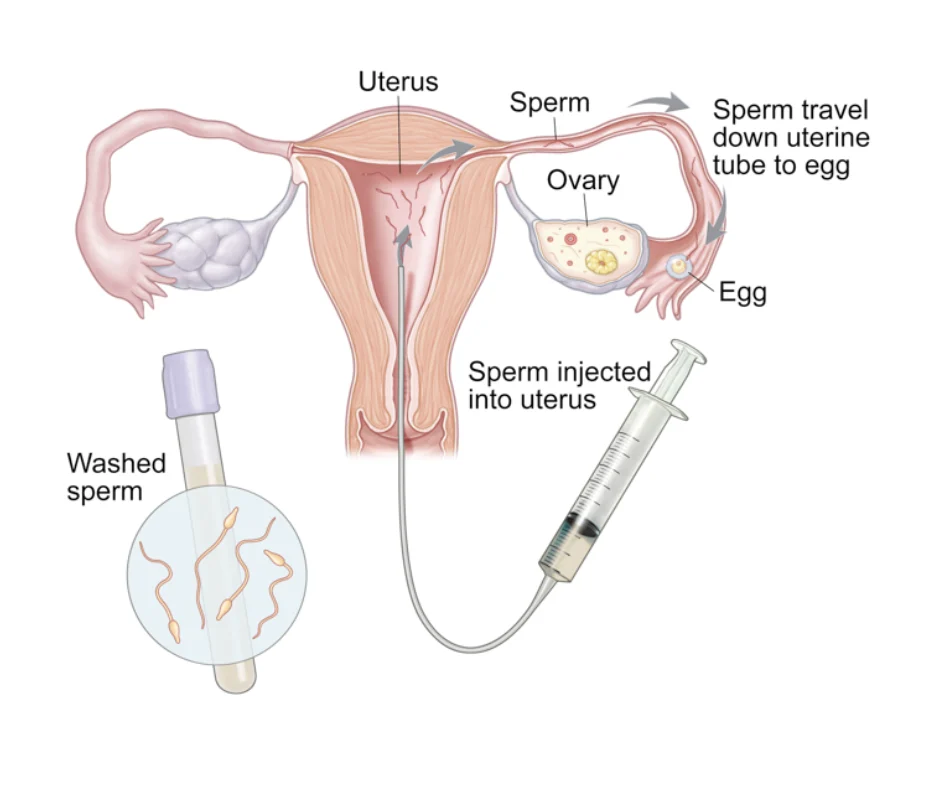
Surgery is another treatment option for couples struggling with fertility issues. The most common surgical procedures for fertility include laparoscopy and hysteroscopy. Laparoscopy is a minimally invasive procedure that involves making small incisions in the abdomen to examine and treat underlying issues such as endometriosis, fibroids, and blocked fallopian tubes. Hysteroscopy, on the other hand, is a procedure that involves inserting a thin, lighted tube through the cervix to examine and treat abnormalities in the uterine cavity.
Pros of Surgery:
1. Higher success rates: Surgery can effectively treat underlying issues that may be causing infertility, leading to higher success rates compared to fertility medications.
2. Can treat structural problems: Surgery can address structural problems such as blocked fallopian tubes, which cannot be treated with fertility medications.
3. Single procedure: Unlike fertility medications, which may require multiple cycles, surgery is a one-time procedure.
Cons of Surgery:
1. Invasive: Surgery is a more invasive option compared to fertility medications, which may require a longer recovery time.
2. Higher costs: Surgical procedures can be expensive, and they may not be covered by insurance, making them less accessible to some couples.
3. Potential risks: As with any surgery, there are potential risks involved, such as bleeding, infection, and damage to surrounding organs.
How to Make an Informed Decision:
1. Understand the cause of your infertility: Before making a decision, it is essential to understand the root cause of your infertility. This will help you determine which treatment option is best for you.
2. Discuss with your doctor: Your doctor can provide you with more information about the risks and benefits of both fertility medications and surgery based on your specific case.
3. Consider your age and overall health: Your age and overall health are important factors to consider when deciding between fertility medications and surgery. Older women may have a lower success rate with fertility medications, while women with certain health conditions may not be suitable candidates for surgery.
4. Discuss the costs: Fertility treatments can be expensive, and it is crucial to consider the costs involved and whether they are covered by insurance.
5. Be open to alternative treatments: In some cases, alternative treatments, such as acupuncture or lifestyle changes, may be beneficial in conjunction with fertility medications or surgery.
In summary, both fertility medications and surgery are viable options for couples struggling with infertility. Fertility medications may be a good first step, as they are non-invasive, cost-effective, and have fewer risks. However, if the underlying cause of infertility is structural, surgery may be a more effective option. Ultimately, it is essential to consult with your doctor and consider all factors before making a decision.